Nervous Patient Dentist in London
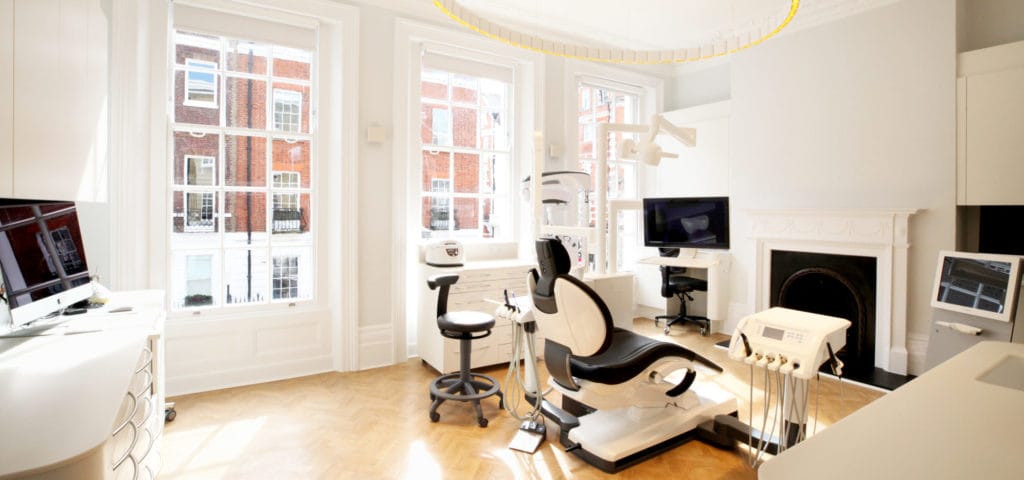
Virtual tour our clinic in advance of your appointment
How do we ease your anxiety
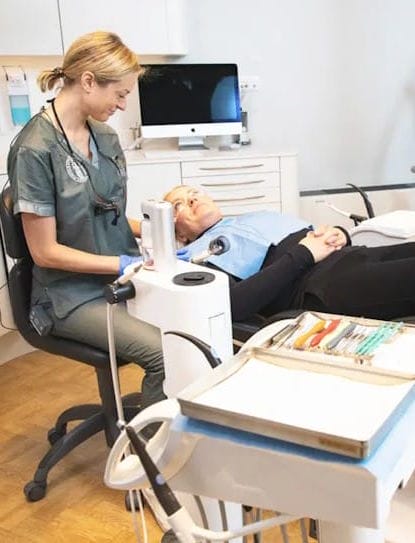
For many people, dental anxiety stems from past experiences — perhaps a painful procedure, a lack of control, or simply fear of the unknown. Others feel nervous because of the sights, sounds, or smells of a clinic.
Whatever the cause, we understand that walking into a dental practice can feel overwhelming. That’s why we’ve designed every detail of our clinic, from our receptionist’s warm welcome to our gentle chairside manner, to make you feel comfortable and stress-free.
Compassionate care for nervous patients
Our philosophy is simple: every patient deserves kindness, understanding, and time.
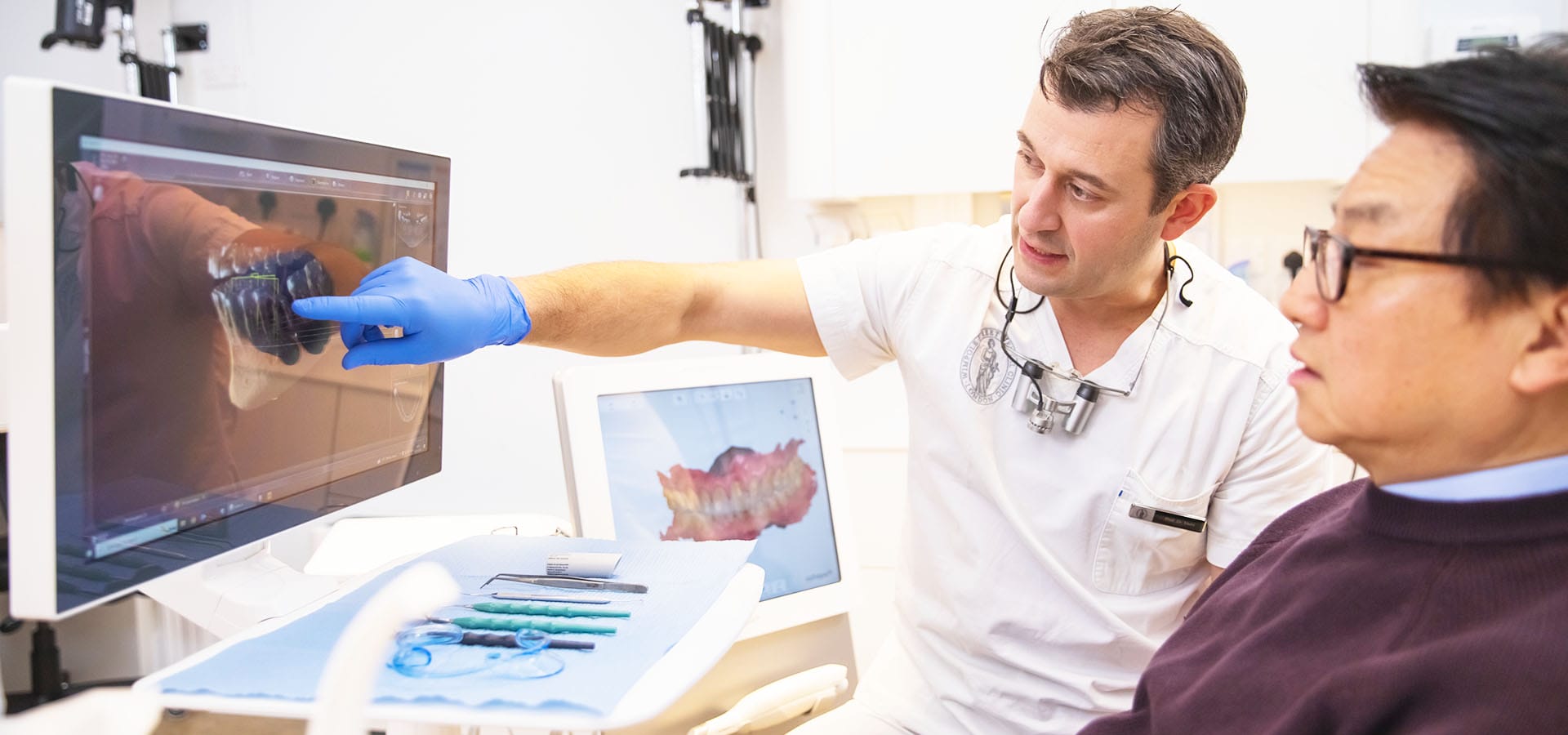
From your very first call, our dental team listens to your concerns and creates a plan tailored to your needs.
We encourage open communication — if something worries you, tell us. Our team will explain each stage clearly, check that you are ready before we begin, and stop whenever you need. That level of compassionate care helps many nervous patients feel safe again.
How do we ease your anxiety
We use a combination of techniques to reduce dental anxiety and promote calm:
- A relaxing environment with soft lighting and music
- Friendly, patient-centred staff from reception to surgery
- Clear explanations to remove uncertainty
- Pain-free injections and modern dental anaesthesia
- Conscious sedation when extra reassurance is needed
- Unhurried appointments with your familiar dentist
Our gentle touch and calm pace are designed to help you relax — so you can focus on your smile, not your fears.
What is conscious sedation?
Conscious sedation allows nervous patients to undergo dental treatment safely and comfortably. You’ll feel deeply relaxed and may even drift in and out of sleep, but you’ll still be able to respond to your dentist when needed.
At Wimpole Street Dental Clinic, our sedationist uses IV conscious sedation, always under full monitoring. You remain pain-free, calm, and unaware of any discomfort during your treatment.
Who can benefit from sedation dentistry?
Conscious sedation is ideal for:
- Dental patients with dental phobia, nerves or extreme anxiety
- Those with a strong gag reflex
- People needing long or complex procedures
- Anyone with sensitive teeth or a low pain threshold
- Patients who have avoided dental care for years
With sedation, you can undergo anything from a root canal to dental implants without fear or discomfort.
What happens during sedation treatment?
- Consultation and assessment – Your dentist reviews your health and discusses your concerns.
- Preparation – The sedationist explains the process and answers all questions.
- Sedation – The medication is given intravenously. Within minutes, you’ll feel deeply relaxed.
- Treatment – Your dentist completes the planned dental work pain-free.
- Recovery – You’ll rest in our recovery area for 10–15 minutes, fully monitored until you’re ready to go home.
You’ll be able to walk, talk, and respond normally — but most patients remember very little about the procedure itself.
Types of dental sedation
There are three levels of sedation dentistry recognised in the UK:
Minimal sedation (anxiolysis)
You stay awake and aware but feel calm and unconcerned. Often used for mild anxiety or simple treatments.
Moderate (conscious) sedation
You become sleepy and relaxed, respond to instructions, and usually won’t remember much. This is the most common option at our clinic.
Deep sedation / general anaesthesia
Reserved for hospitals only. It is not permitted in standard dental surgeries in the UK.
Preparing for sedation dentistry
Before your appointment, you’ll receive clear instructions. In most cases:
- Avoid solid food for six hours before treatment
- Clear liquids (like water) are allowed up to two hours before
- Let your dentist know if you take medication or have diabetes
- Arrange for a friend or relative to accompany you home
These steps ensure your safety and comfort before, during, and after your visit.
What treatments can be done under sedation?
Almost every dental treatment can be performed comfortably under sedation, including:
- Hygiene appointments and routine dental care
- Fillings, crowns, and veneers
- Root canal treatments
- Dental implants or bone grafting
- Cosmetic and restorative procedures
Our nervous patient dentist team will help you choose the right level of sedation for your needs.
Meet your award-winning Nervous Patients dentist and team…
We’ve helped thousands of patients who once avoided dentists completely due to fear or trauma. Our approach rebuilds trust through honesty, empathy, and respect. Many patients tell us that their first appointment, whether general or cosmetic dentistry, was the first time they’ve ever felt relaxed in a dental chair.
At Wimpole Street Dental Clinic we know that visiting the dentist can be stressful, especially if you’re anxious about treatment. That’s why our dedicated sedation team – led by experts such as Dr Andre du Plessis and Dr Etienne Deysel – are here to gently support you through your experience.
Using the latest sedation techniques, they work alongside our clinical team to ensure your journey is as calm and pain-free as possible. Whether you’re here for routine work or something more advanced, you can rest assured that your comfort and peace of mind are our top priority.







Restoring confidence in your smile and dental care
Dental anxiety shouldn’t stop you from having a healthy, confident smile. Whether you’ve delayed treatment for years or are facing a complex procedure, we’ll guide you gently through each step.
With our compassionate care, sedation options, and patient-first philosophy, you can finally enjoy a stress-free dental experience.
When to talk to your dentist
If you’ve been avoiding appointments, are struggling with dental phobia, or simply want to know your options, book a consultation. Our dental team will listen carefully, explain your choices, and help you find the best approach to ease your anxiety.
Nervous Patient FAQs
Wimpole Street Dental Clinic is led by world-class clinicians with decades of experience in advanced restorative and surgical dentistry. Our dentists have performed over 1,200 sedation-assisted procedures, giving us unparalleled expertise in caring for anxious patients. Every member of our team — from our reception staff to our sedationist — is trained to deliver calm, compassionate care using the most advanced techniques available in modern dentistry.
Our commitment to comfort, safety, and clinical excellence makes us the preferred clinic for discerning patients seeking a truly high-end dental experience in London.
Sedation dentistry uses carefully monitored medication to help you relax and feel calm while remaining awake and responsive. You’ll be able to communicate with your dentist, but most patients remember very little of the treatment afterwards.
General anaesthesia, by contrast, induces complete unconsciousness and is only permitted in hospital environments. At Wimpole Street Dental Clinic, we exclusively use conscious sedation — a refined, safe, and medically supervised method offering exceptional comfort with rapid recovery.
Yes. Conscious sedation is an extremely safe and well-established procedure, particularly when performed by experienced professionals. At our clinic, sedation is overseen by a qualified medical sedationist who continuously monitors your breathing, blood pressure, and oxygen levels throughout your treatment.
Our dentists are trained in advanced sedation protocols, ensuring you remain comfortable and completely safe at every stage. With decades of clinical experience, we have refined our process to the highest international standards.
Yes. Most dental treatments, including dental implants, root canal therapy, crown placement, and cosmetic procedures, can be carried out under sedation.
This allows nervous patients to undergo complex or lengthy treatments in total comfort. At Wimpole Street Dental Clinic, our expertise in implant surgery, aesthetic restorations, and advanced reconstructive dentistry ensures that sedation is seamlessly integrated into even the most sophisticated procedures.
Our dentists and sedationists have collectively performed over 1,200 sedation treatments for patients with varying degrees of dental anxiety.
We are one of the few clinics in London where specialist-led care combines clinical excellence with an unparalleled focus on patient comfort. Our team’s advanced training, both in the UK and internationally, ensures you’re cared for by experts with decades of combined experience in complex and anxiety-sensitive dentistry.
You’ll feel deeply relaxed, calm, and detached from the dental procedure. Many patients describe the experience as peaceful, as if time passes quickly. You’ll be aware enough to respond to gentle questions but won’t feel pain or discomfort.
Our sedationist remains by your side throughout, monitoring your wellbeing with the precision and professionalism that define our clinic’s standards of care.
Recovery is typically quick — most patients feel alert again within 10–15 minutes after treatment. You’ll rest briefly in our comfortable recovery area before leaving the clinic, accompanied by a friend or relative.
Because the effects wear off gradually, you may feel pleasantly drowsy for a few hours, so it’s best to rest at home for the remainder of the day. Our team provides full post-sedation guidance and remains available should you have any questions.
We understand that previous experiences can have a lasting emotional impact. Many of our patients come to us after years of avoiding dentistry altogether.
At Wimpole Street Dental Clinic, you’ll never be rushed or judged. Our approach is built around trust, respect, and open communication. Every detail of your care — from the first consultation to the final follow-up — is managed with discretion, empathy, and clinical precision. Over time, most of our patients rediscover confidence and even enjoyment in caring for their smile.
Not necessarily. For some anxious patients, sedation is an initial step to rebuild confidence and restore oral health.
As trust grows and positive experiences replace fear, many patients find they no longer need sedation for routine appointments. Our goal is always to help you regain control of your dental wellbeing in a way that feels empowering, not dependent.
Every detail of our London dental practice has been designed with patient comfort in mind — from our tranquil reception space and soothing lighting to our private treatment rooms equipped with state-of-the-art technology.
Our team’s calm, respectful manner and meticulous attention to detail reflect the clinic’s ethos: that world-class dentistry should be as comfortable and reassuring as it is clinically advanced.
We offer gentle solutions for younger patients who experience dental anxiety, but IV sedation is typically reserved for adults. For children, we focus on creating a positive, confidence-building experience using communication, relaxation techniques, and local anaesthesia where needed. If sedation is appropriate, our clinicians will discuss safe, tailored options with parents or guardians.
Simply contact our friendly reception team, who will guide you through the process. We recommend scheduling an initial consultation, during which our dentists will assess your needs, review your medical history, and explain all options for anxiety-free care.
You’ll leave your consultation with a clear, bespoke plan for comfortable, pain-free treatment — handled with the precision and discretion that define Wimpole Street Dental Clinic.
Content updated
Written by: Prof Dr Christian Mehl
Medically reviewed by: Dr Raul Costa
New page content
Written by: Prof Dr Christian Mehl
Medically reviewed by: Dr Raul Costa
New page design
Written by: Prof Dr Christian Mehl
Medically reviewed by: Dr Raul Costa
Original content created
Written by: Prof Dr Christian Mehl
Medically reviewed by: Dr Raul Costa
Wimpole St Dental Clinic has strict sourcing guidelines and relies on peer-reviewed studies, academic research institutions, and medical associations. We avoid using tertiary references. You can learn more about how we ensure our content is accurate and current by reading our editorial policy.