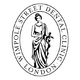Root Canal Treatment in London
Saving a decaying tooth doesn’t have to be intimidating. Thankfully, the experienced professionals at Wimpole Street Dental Clinic in London can provide the utmost quality of care to conserve your smile.

Treatment
60 - 120 minutes

Price
From £1,100

Team Experience
40+ years

Recovery Time
1 day

Google Rating
★★★★★ (4.9)
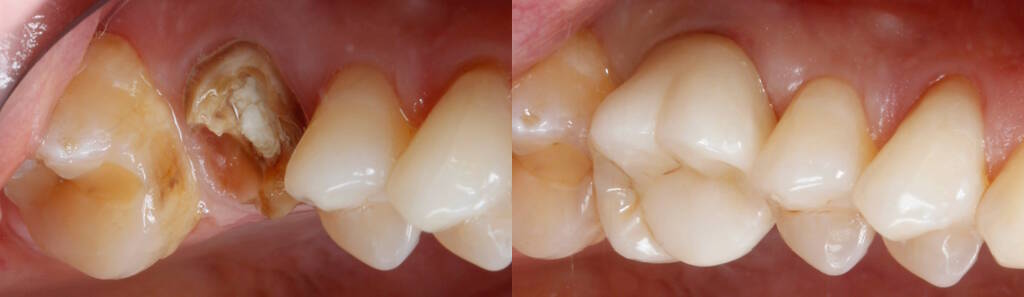
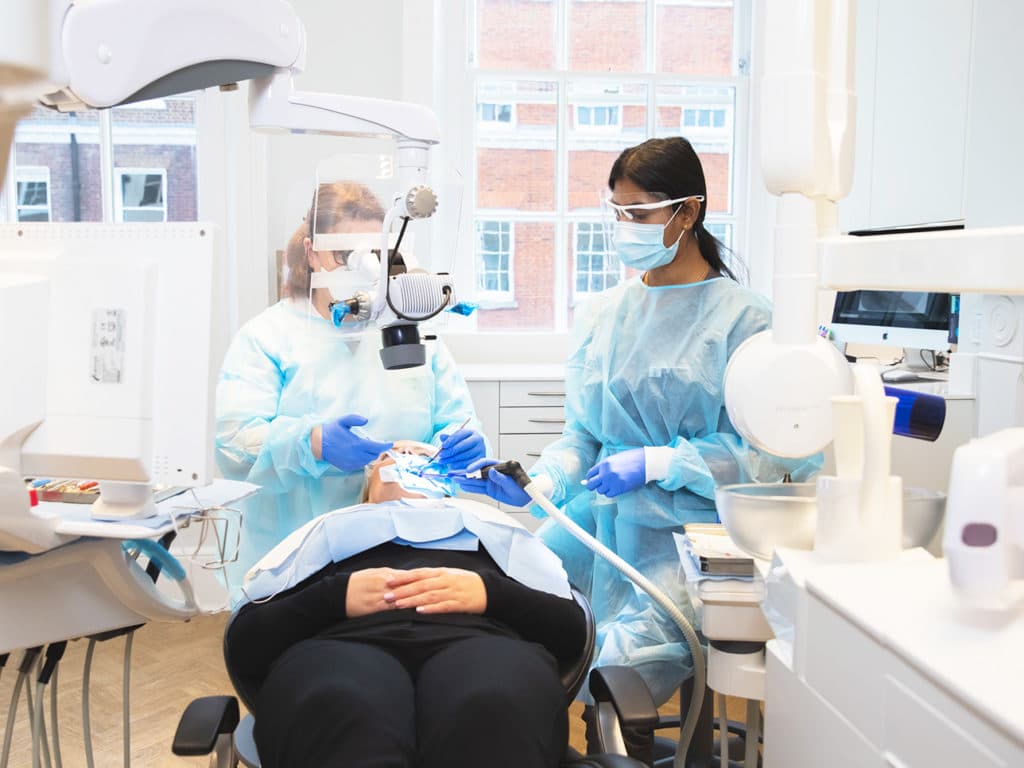
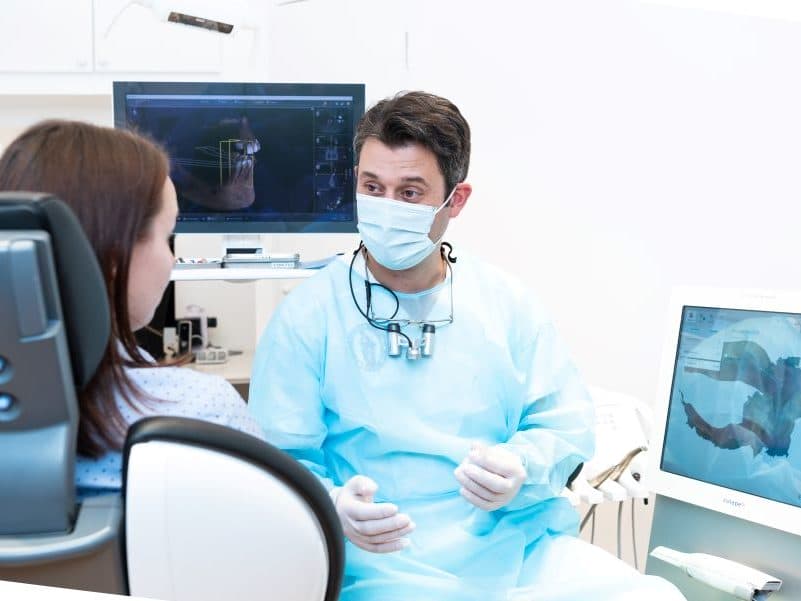
Examples of root canal treatment

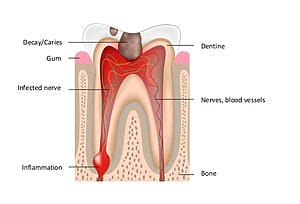
As dental patients, we all understand what it means to experience a severe toothache and do not always understand the reason why. Root canal pain can be caused by inflammation or damage to the root of the tooth that ultimately leads to infection of the tooth and pulp. As our clinical priority at Wimpole Street Dental Clinic is on saving teeth wherever possible, root canal treatment presents an effective and virtually pain-free but necessary opportunity to do this.
The root canal pain and/or discomfort you may be experiencing can cause a ringing, piercing pain in the tooth or perhaps a dull, pulsating sensation. It is prudent for us to act fast to cleanse and disinfect the root canal and surrounding gums of any bacteria, fill and seal the area in order to strengthen the tooth and restore you and your teeth to the comfort and confidence of your natural smile as soon as possible.
Many patients are able to get back to normal straight away, though they may experience some slight sensitivity following the endodontic treatment.
Who is suitable for Root Canal?
At Wimpole Street Dental Clinic, when you attend your appointment, we conduct an initial consultation with you to identify the tooth affected, discover the extent of the proposed root canal treatment required and its potential complexity, and so guide our optimal choice of the dental care plan for you.
If there is a good chance of saving the tooth and the patient’s oral health is otherwise in good condition, we may recommend a course of endodontic treatment such as a root canal.
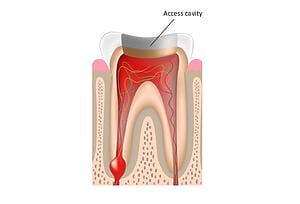
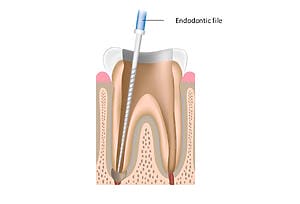
What happens during Root Canal Treatment?
Remember that once root canal treatment begins, you will receive a local anaesthetic to numb the infected tooth and surrounding gum,s ensuring you experience a virtually pain-free appointment with us. In terms of pain after root canal, dental patients may only experience minor sensitivity to the tooth in question for a few days afterwards.
Here at Wimpole Street Dental Clinic, we can offer our dental patients video glasses so you can relax by watching a film or television show of your choice as we conduct this procedure for you. Root canal treatment can often be completed in just one visit to us so do not hesitate to book this kind of appointment designed to safeguard your smile and your health.
Advanced/Related Root Canal Treatments
Apicectomy
If a previous root canal hasn’t fully resolved the problem, an apicectomy may be recommended. This is a minor surgical procedure that removes the tip of the tooth root and any surrounding infected tissue to help save the tooth. It’s typically used when retreatment isn’t possible or hasn’t been successful. Learn more about apicectomy.
Root canal retreatment
Sometimes, a tooth that’s had root canal treatment can become painful or infected again. Root canal retreatment gives the tooth a second chance by carefully removing the old filling material, disinfecting the canals, and resealing the tooth. This treatment is ideal for patients whose previous root canal has failed or developed new issues. Learn more about root canal retreatment.
Vital pulp therapy
Vital pulp therapy is a gentle alternative to full root canal treatment, aimed at preserving the healthy part of the tooth’s pulp. It’s especially suitable for younger patients or cases where the damage hasn’t spread throughout the tooth. By keeping the living tissue intact, this approach helps the tooth continue to develop and stay strong. Learn more about vital pulp therapy.
A brief summary of Root Canal Treatment
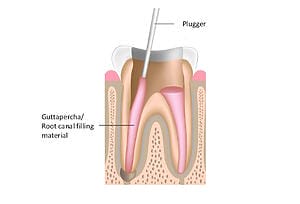
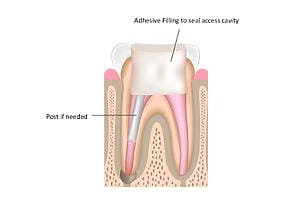
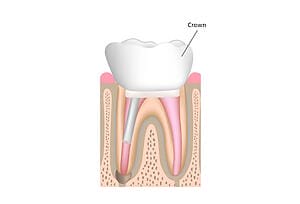
Meet your award-winning Root Canal Treatment dentist and team…
- We have over 75+ years of combined dentistry experience across our specialist team.
- 10,000+ treatments performed and counting.
- We are leaders in the dental industry – we regularly teach, lecture and publish our research work internationally.
Our Expertise
Whenever you need to take care of your smile – in an emergency, during routine care or when booking cosmetic dentistry – you naturally seek a qualified, skilled and experienced dental professional whom you can trust to deliver the premium dental care you expect at every appointment.
We would like you to consider placing your trust in Wimpole Street Dental Clinic because:
We are internationally renowned within the dental profession.
We pride ourselves on offering evidence-based dentistry with a person-centred approach.
We use a microscope or other magnifying equipment to ensure world-class results.
We offer a new standard in modern specialist dentistry in our clinical methodology – leveraging the optimal combination of the finest handcraft, digital computer-aided design (CAD) and computer-aided manufacturing (CAM) technology to deliver excellence in both patient care and dental treatment success.
We perform all root canal treatments in accordance with the guidelines of the German and British Society of Endodontics here at Wimpole Street Dental Clinic in London.
Root canal for nervous patients
Patients who are particularly worried about root canal treatment can undergo this dental treatment under light or deep sedation if they would prefer not to experience the entire dental procedure under just local anaesthesia.
Root canal treatment is often a long procedure, and as such, many patients dread having to spend too much time sitting in a chair. To help avert boredom and help distract you during the root canal procedure, we provide video glasses so you can relax and watch a film or television show of your choice.
Take your first step with Wimpole Street Dental Clinic
Discover the path to a brighter smile with Wimpole Street Dental Clinic! Our team of skilled professionals utilises advanced technology to provide personalised dental care in a comfortable setting.







Merged Retreatment, Apicectomy and Vital Pulp Therapy into one page
Written by: Prof Dr Christian Mehl
Medically reviewed by: Dr Raul Costa
New page design
Written by: Prof Dr Christian Mehl
Medically reviewed by: Dr Raul Costa
Author biography added
Written by: Prof Dr Christian Mehl
Medically reviewed by: Dr Raul Costa
Original content created
Written by: Prof Dr Christian Mehl
Medically reviewed by: Dr Raul Costa
Wimpole St Dental Clinic has strict sourcing guidelines and relies on peer-reviewed studies, academic research institutions, and medical associations. We avoid using tertiary references. You can learn more about how we ensure our content is accurate and current by reading our editorial policy.
- Lumley PJ, Adams N, Tomson P. Root canal retreatment. Dent Update. 2006 Nov;33(9):518-20, 522-4, 526-8, 530. doi: 10.12968/denu.2006.33.9.518. PMID: 17176738.
- Ford TR, Rhodes JS. Root canal retreatment: 2. Practical solutions. Dent Update. 2004 Mar;31(2):97-102. doi: 10.12968/denu.2004.31.2.97. PMID: 15065373.
- Tang L, Sun TQ, Gao XJ, Zhou XD, Huang DM. Tooth anatomy risk factors influencing root canal working length accessibility. Int J Oral Sci. 2011 Jul;3(3):135-40. doi: 10.4248/IJOS11050. PMID: 21789962; PMCID: PMC3470095.
- Rabinovich IM, Abakarova DS, Snegirev MV. [Root canal irrigation – component of endodontic treatment success]. Stomatologiia (Mosk). 2011;90(3):80-3. Russian. PMID: 21845784.
- Tidmarsh BG. Preparation of the root canal. Int Endod J. 1982 Apr;15(2):53-61. doi: 10.1111/j.1365-2591.1982.tb01341.x. PMID: 6951816.