Bone grafting for dental implants in London
Bone augmentation is necessary in cases where the volume of the jawbone is not sufficient for an implant. It can be performed on both the upper and lower jaw and ensures that dental implants can be securely anchored. We often mix the patient’s bone with an artificial bone to restore the original contour of the jawbone and embed the implant for long term success.

Treatment
1+ hours

Price
From £800

Team Experience
50+ years

Recovery Time
7+ days

Google Rating
★★★★★ (4.9)

When a patient loses a tooth, or, even worse, several teeth, the bone in that area will shrink considerably. This will have a tremendous impact in case the patient then wants to restore the missing tooth or teeth, whether with a dental implant or a bridge.
In these cases, bone grafting prior to implant placement may be required in order to achieve a predictable, stable, easy to maintain and more aesthetic outcome.
What is bone grafting?
Bone grafting (bone augmentation) is the transfer of bone tissue from another location within the body (autogenous bone), the insertion of a natural replacement material (allogenic bone) or even the use of a synthetic tissue (artificial, also called xenogenic, bone) to an oral site where it is needed after bone volume loss. It is also possible to blend a patient’s bone with a natural or artificial bone resource to restore the original contour of the jawbone and so prepare for a dental implant.
This surgery can be necessary if an implant is needed, but the current volume of your jawbone is not strong enough to support one if fitted. Bone grafting can be performed on the upper or lower jaws and is often conducted on an outpatient basis, under local anaesthetic or light sedation, at our clinic in Wimpole Street, central London.
If comprehensive bone augmentation with bone extraction from the pelvis is advised, please note that this is not conducted under normal sedation in our clinic. Usually, the range of bone grafting procedures offered in our clinic, from the straightforward to the more complex, is enough to solve 99.9 % of all implant and bone augmentation cases.
Meet your award-winning Bone Grafting dentist and team…
- We have over 75+ years of combined dentistry experience across our specialist team.
- 10,000+ treatments performed and counting.
- We are leaders in the dental industry – we regularly teach, lecture and publish our research work internationally.
Our Expertise
We believe we offer the perfect balance of location, professional expertise and digitally enabled dentistry on an in-house basis, should you need our bone grafting techniques to restore your oral health. We are delighted to have Prof Dr Christian Mehl, who has vast experience in bone augmentation surgery, at our clinic.
We genuinely appreciate that the decision to proceed with a dental implant is one to consider, and should you need bone augmentation in order for the implant to succeed, you may need more time, information and reassurance that you have chosen the right dental clinic to perform this surgery. Trust that we have all the resources on hand to meet and even exceed your care expectations.
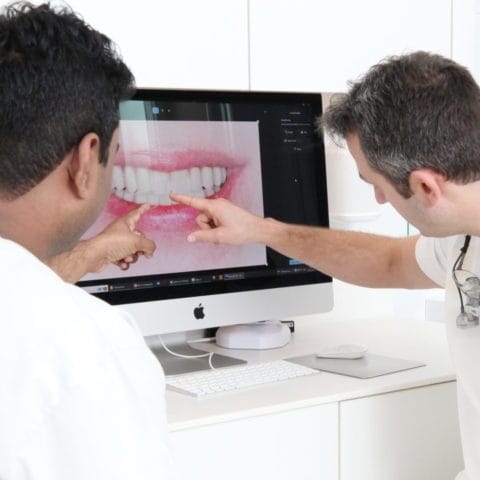
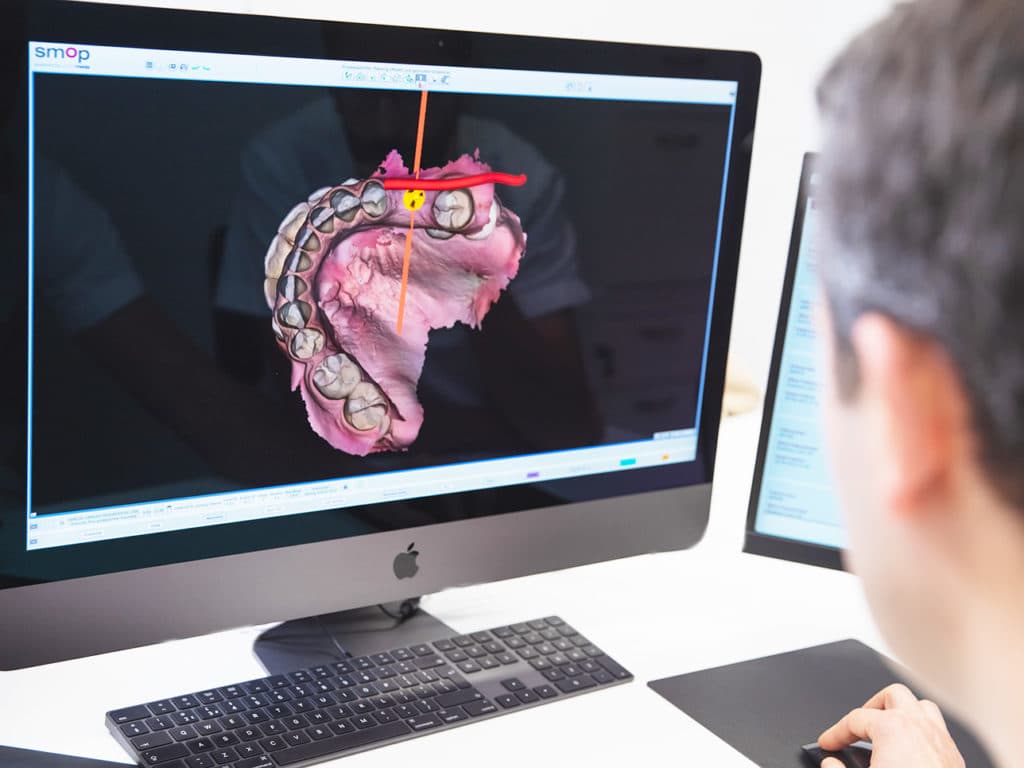
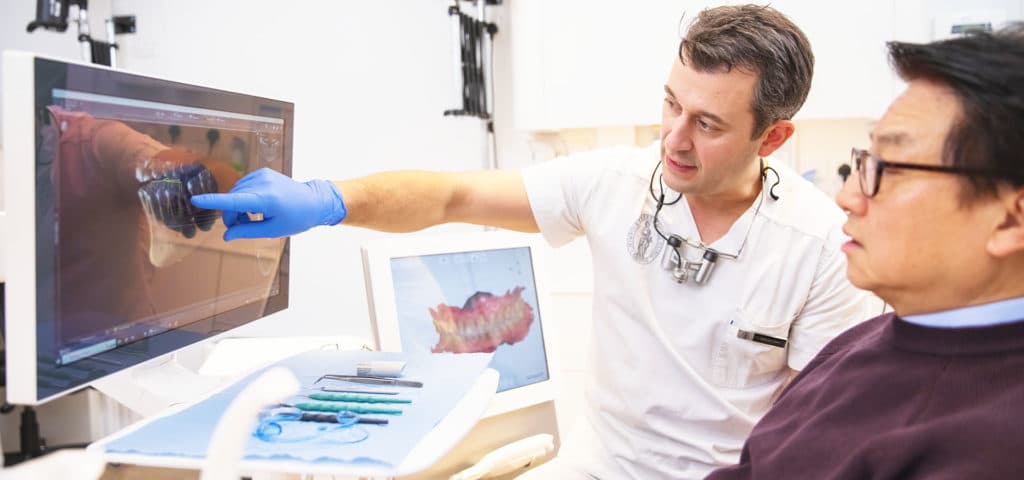
From the moment you contact us to your first consultation and onto your first surgical appointment, our digital workflow principles mean every expert involved is aware of your exact case. Plus, we confidently employ ultrasound-driven bone surgery (or Piezoelectric surgery) to work precisely, effectively and efficiently to deliver with the utmost care the bone augmentation you need.

Helen Li
Wimpole Street Dental has the highest most ethical standard of work, personable approach, clear and safe procedures, top notch excellence and reliability in treatment provided with utmost professionalism from crème de la crème world class specialists all under one roof.
Who is suitable for bone grafting?
Patients recommended for a dental implant who are in good general and good oral health but require more jawbone support, may present as suitable candidates.
Bone grafting for this purpose is needed if there is less than about 2 mm of bone present on all sides of the proposed dental implant site. Bone grafting is vital where the body naturally reduces the bone volume in the jaw area once the tooth is lost, and where the implant is now recommended.
Why not contact us today if you are thinking about this procedure?
Take your first step with Wimpole Street Dental Clinic
Discover the path to a brighter smile with Wimpole Street Dental Clinic! Our team of skilled professionals utilises advanced technology to provide personalised dental care in a comfortable setting.




New page design
Written by: Prof Dr Christian Mehl
Medically reviewed by: Dr Raul Costa
Author biography added
Written by: Prof Dr Christian Mehl
Medically reviewed by: Dr Raul Costa
Original content created
Written by: Prof Dr Christian Mehl
Medically reviewed by: Dr Raul Costa
Wimpole St Dental Clinic has strict sourcing guidelines and relies on peer-reviewed studies, academic research institutions, and medical associations. We avoid using tertiary references. You can learn more about how we ensure our content is accurate and current by reading our editorial policy.
- Mehl C, Kern M, Zimmermann A, Harder S, Huth S, Selhuber-Unkel C. Impact of Cleaning Procedures on Adhesion of Living Cells to Three Abutment Materials. Int J Oral Maxillofac Implants. 2017 Sep/Oct;32(5):976-984. doi: 10.11607/jomi.5630. PMID: 28906501.